 Biliopancreatic Diversion (BPD) creates a smaller stomach (similar to gastric bypass surgery), but in addition there is less absorption of ingested food inside the intestine (malabsorption).
Biliopancreatic Diversion (BPD) creates a smaller stomach (similar to gastric bypass surgery), but in addition there is less absorption of ingested food inside the intestine (malabsorption).
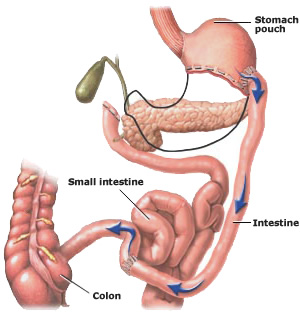
Biliopancreatic diversion changes the normal process of digestion by making the stomach smaller and allowing food to bypass part of the small intestine so that patients absorb fewer calories. A portion of the stomach is removed entirely, creating a smaller stomach pouch. The distal part of the small intestine is then connected to the pouch. Like gastric bypass surgery, this type of operation has the potential for developing nutritional deficiencies.
Biliopancreatic diversion is becoming less common compared to other types of bariatric surgery, in large part because of the need for more extensive nutritional follow-up and long-term monitoring.
Our surgeons are ready to help you decide which bariatric procedure is right for you.
Biliopancreatic Diversion Modifications
Some surgeons have modified the standard BPD operation to further reduce stomach capacity in the heaviest patients (those with a BMI 50 or more). Some surgeons have also lengthened the common channel in less obese patients (BMI 40-50) to reduce the incidence of malabsorption-related complications. This has become known as biliopancreatic diversion with duodenal switch. This “duodenal switch” is so named because the functional portion of the duodenum (the upper small intestine) is bypassed from digestive continuity in a reversal or “switch” technique.
Is biliopancreatic diversion reversible?
Yes and no. The malabsorptive part of the procedure can be reversed. In around 2% of patients, there is severe malabsorption and nutritional deficiency that requires restoration of the normal absorption.
