
PMC's special team of board certified physicians, specialists and nurses provides prompt, quality care to heart attack patients, including critical life-saving treatments such as emergency angioplasty and therapeutic hypothermia.
Emergency angioplasty is a life-saving procedure that is used to treat patients who are suffering certain acute myocardial infarctions (heart attacks). Performed by PMC's board certified interventional cardiologists, this procedure is used to open clogged arteries in response to a heart attack. Emergency angioplasty quickly increases the flow of blood and oxygen through blocked arteries without the need for invasive heart surgery. Only state-licensed facilities, like PMC, can offer this procedure, which has been proven to reduce mortality rates in heart attack patients.
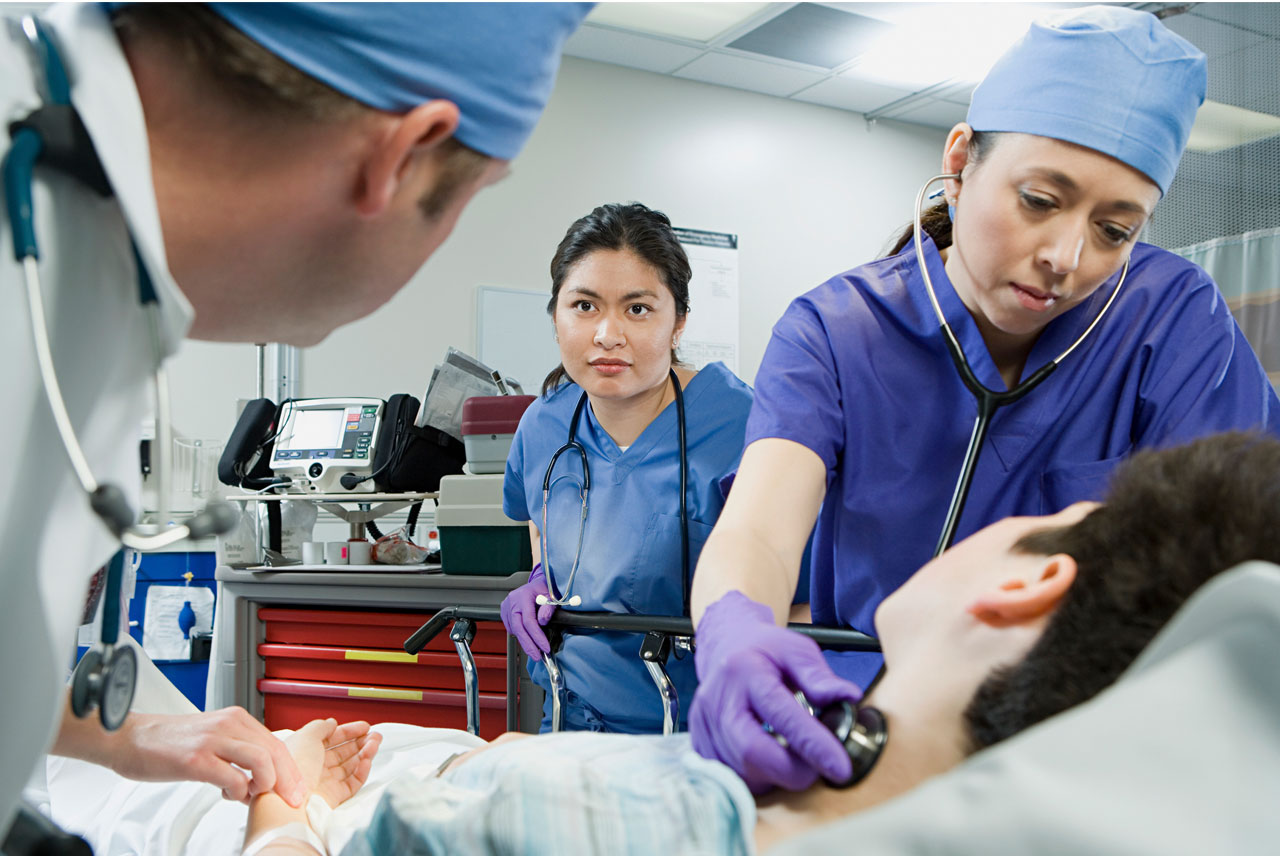
Timing is critical, and reducing the time between patients' arrival in the Center for Emergency Care and the emergency angioplasty procedure (“door-to-balloon” times) can have dramatic effects on patient outcomes. In 2013 at PMC, the door-to-balloon time was reduced to an average of 86 minutes – a figure that falls within the 90 minutes or less recommended by the American College of Cardiology (ACC) and the American Heart Association (AHA) guidelines. To support timely treatment for heart attack patients, PMC has implemented core strategies recommended by the Door-to-Balloon (D2B) Alliance campaign, which is sponsored by the American College of Cardiology and 38 partner organizations. Also, through PMC's LIFENET Cardiac Care System, which transmits EKG data to emergency physicians and staff while patients are in transit to the hospital, the hospital's board certified emergency physicians and interventional cardiologists are prepared to initiate this critical, lifesaving service even more promptly.
In the event a patient needs open heart surgery, PMC has an emergency transport team on site to immediately transfer the patient to the Heart Center of New Jersey at Robert Wood Johnson University Hospital in New Brunswick.
Studies suggest that patients treated with emergency angioplasty rather than clot-dissolving drugs have a higher survival rate and are more likely to survive another heart attack if one occurs. Emergency angioplasty has been found to reduce the risk of heart attack-related complications – including stroke or a second heart attack – and reduce the likelihood of the development of congestive heart failure due to muscle damage. In most cases, emergency angioplasty requires only local anesthesia, reducing the risk of related complications.
In 2009, PMC began offering therapeutic hypothermia – a relatively new advancement that improves heart attack survival, reducing the chance of brain damage and giving patients a better chance at full recovery. This technique – which should be administered within six hours of cardiac arrest – lowers the body's temperature and helps slow the chemical processes that occur when the brain is deprived of oxygen, thereby helping protect fragile brain cells and neurological processes.
Therapeutic hypothermia is used for a very select group of patients; however, for those patients, it can make the difference between life and death.
Additional information about heart attacks is available by visiting the American Heart Association's website.
